On this page: ➊ Screening・➋ Counselling
Hepatitis C testing HCV
1. Screening
Early detection and treatment are key to keeping the overall cost low, whether that cost be measured in human suffering, lost opportunity, preventable health consequences, avoidable infections, or money.
The cost of not knowing
The cost of diagnosis and treatment of hepatitis C has fallen dramatically, but for a health system, the costs still add up. However, the cost of not diagnosing and treating are much higher. Calculate the cost of diagnosis and treatment, with results given in monetary and quality-adjusted life years.
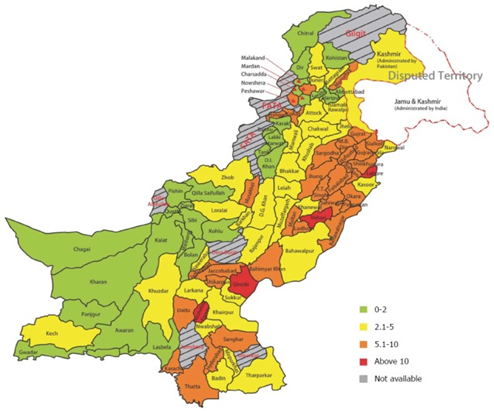
The cost of HCV screening – An example of Pakistan
Hepatitis C is most reliably diagnosed by detection of RNA in the blood. However, as this test takes preparation and analysis time, in most circumstances people are first screened to see if they have antibodies to hepatitis C to see if they have been exposed to hepatitis C, and blood for the next test is collected from those who have.
The most efficient way to do this is with a rapid test for HCV antibodies, which takes only one drop of blood, and gives a result in 5-20 minutes. These tests can be given at the community level by workers after a short training session. The WHO has assessed some of these tests, and the sensitivity and specificity of many are near 100%, and some cost less than US$1. The tested person can usually wait to get the results and counselling. Part of the counselling for those who test positive is to do a further test.
The screening test alone does not tell whether someone has active infection. Anyone who has ever been exposed to hepatitis C, whether their immune system overcame the infection, or whether they were treated and cured, will test positive on this kind of test. The second step in diagnosis is to test the blood for viral RNA with a PCR test. This shows whether the virus is present in the blood. This test needs a larger volume of blood to test, and as the analysis takes some hours for the analysis, the results are usually given on a subsequent appointment.
Counselling micro-elimination
2. Counselling
In this section you will find advice on:
1. Pre-screening counselling
2. Post-screening counselling, positive and negative test
3. Pre-confirmatory counselling
4. Post-confirmatory counselling, positive and negative test
These counselling guidelines are intended for trained lay counsellors, and so are quite general. As with all counselling, they need to be adapted to the context and project. They goals for the general counselling are to give an optimistic message that will help people move from their level of knowledge to greater awareness and most important, to action. This approach must also address any stigma in the community.
Lay counselling is a support for counselling by a prescribing healthcare provider, and not a substitute for it. With good counselling in several phases before, a new patient should be better able to understand and retain information when starting treatment. With a better knowledge base, the patient can also ask relevant questions at that time, and advocate for themselves.
No one should be left shocked and panicked by their test results. Counselling is key to setting the test results in perspective — whether positive or negative — and should let people know the next steps they can take if they test positive, before they even get tested. Counselling is not only about you giving information. It is also an excellent opportunity for you to learn about the lives and thoughts of your audience.
Even if you are from the same community as the group, you are likely still different because of your interest and training in health. You can learn about the understandings of hepatitis, including what people know, do not know, and mistaken beliefs. These will all help you improve the counselling and health education materials.
Counselling must be sensitively adapted to the context, including culture, health economics, education, and the common health issues and risk behaviours seen in that time, place, and particular population. Knowing the specific stigmas in the community and the beliefs or values they rest on will help you dismantle them.
Ideally, people getting counselling should have already have at least basic information about hepatitis. This could be one information session on hepatitis C, informing them about the basics of the disease, risk factors, cultural issues, prevalence in the area or country, and so on. In many real-world cases, this is not so. If the group knows almost nothing about hepatitis C, include these basics and information about treatment, and the services available to them. If it is possible to give an information session at least one day earlier than the counselling and testing, this will give people time to think and talk over the information. They will come to the counselling with better questions, and have better comprehension. Testing requires informed consent. The consent will be better informed if the people have time to think over the information session.
Pre-test hepatitis C counselling, screening test
Pre-test counselling, screening test
Pre-test counselling may be done with individuals or groups. It is the only counselling which can be done in groups without previous informed consent from all participants.
Start by introducing yourself, why you are there, who you are working with, and outlining what you will tell them and how long it will take. The rest of the counselling may be very different according to the knowledge level, the amount of time you have, the size of the group, and any constraints you have. This responsiveness is why counselling in person is better than showing videos or other generic health education materials. Be sure to be as responsive as you can, and to make notes for yourself or your team about any interesting points.
Be aware of whether the person needs more information or less. If they have been tested before, or have a friend or family member with hepatitis C, they may know quite a lot. At a minimum, the first counselling should contain the following points:
- The rapid test is very simple and easy, and does not hurt much. It is just a fingerprick. You will have the results in about 15 minutes.
- Testing is voluntary. You can change your mind at any time.
- Most people with hepatitis C infection feel fine and have no symptoms. That is why the test is important — it is the only way for you to find out early if you have hepatitis C.
- Results are confidential. We will inform only you of the results. Do not ask others about their results. No one has the right to know about your results except you. [Adapt this if there is a reporting requirement.]
- This test will show only if you have ever had a hepatitis C infection. It will not show if you still have an infection now. That needs a second test, which takes a little longer.
- There is no vaccine for hepatitis C.
Depending on how many people there are and how much they know, you may want to review the ways to hepatitis C can be transmitted, preferably by asking them. Affirm the correct ones, possibly with some more detail. Correct the incorrect ones, gently, with more information. Also:
- What would you do if you found out you have hepatitis C?
- Do you have social support?
- (If individual session) Have you been tested for hepatitis C before?
back to Counselling
Post-test HCV counselling, screening test
Post-test counselling, screening test
Whether the test is positive or negative, the results must be given directly to the person confidentially, and with counselling. If they have questions you can answer, answer them right away, before going on. If you cannot answer the question, tell them you will get the answer, and continue. Note the question. If they can wait at the end of the counselling session, and there is someone nearby who will know the answer, or you have a reliable website where you can find the answer, ask them to wait and get the answer. If they cannot wait or you cannot get a reliable answer quickly, ask if they would like you to conact them with the answer, or if they would like to contact you, and give or take phone numbers as needed.
A person with negative results is in a very receptive state of mind for health education. Do not overwhelm them with facts. Here is a sample script. Do not use this script strictly — adapt it to your context, and the particular person. If someone seems knowledgable, ask them about what they know and only fill in where necessary, making sure all important points are covered.
“I am glad to tell you that your test result shows that you have not been exposed to hepatitis C. This is good news, but remember there is no vaccine against hepatitis C, so it is important to keep yourself safe in the future too. In our area, the main risks are [fill in the main risks from your context here]. In general, be aware that any direct contact other people’s blood should be avoided. That includes very small amounts of blood, too small to see, for example on razors and needles. If you do get someone’s blood on your skin or in your eyes or mouth, wash it with water and mild soap. If you think you have been exposed to hepatitis C, wait about one and a half months to get tested. The virus will not do your liver harm in that short time. It takes a while for the results to be able to show up on a test.
“Your hepatitis C test results are confidential. We will not release your results without your authorisation. You can tell whoever you like, but you should not ask other people their results.”
If they or someone in their household can read, provide them with written material about hepatitis risks and prevention.
A person with positive results need to be reassured that this does not mean they currently have an infection of hepatitis C virus — only that they have been exposed. Following is a sample script. Do not stick strictly to the script. Adapt it to your context.
“Your test results show that you have been exposed to hepatitis C. About a quarter of people who have been exposed to hepatitis C clear the infection on their own, without medicines. Usually they clear the infection within a few months. A further test is needed to find out whether you still have the virus or not.”
[Here, you need to tell them how to get a confirmatory test. You may be able to take a blood sample right away, if they consent. Or you can advise them where to go, or make an appointment for them.]
“Don’t worry too much. Even if you have hepatitis C infection, there are good medicines, oral medicines, that cure almost all patients within a few months. If you are confirmed as having hepatitis C infection, we will tell you more about those medicines.
“Whether you have an infection or not, you should be careful not to be exposed to hepatitis C again. Unlike many viruses, hepatitis C can infect you more than once, even if you have cleared the virus or been cured. Also be careful not to expose anyone else. In our area, the main risks are [fill in the main risks from your context here].
In general, any direct contact other people’s blood should be avoided. That includes very small amounts of blood, too small to see, for example on razors and needles. If you do get someone’s blood on your skin or in your eyes or mouth, wash it with water and regular soap.
If you think you have been exposed to hepatitis C, wait about one and a half months to get tested. It takes a while for the results to be able to show up on a test. The virus will not do your liver harm in that short time.
“Your hepatitis C test results are confidential. We will not release your results without your authorisation. You can tell whoever you like, but you should not ask other people their results.”
back to Counselling
Pre-test counselling, confirmatory test for hepatitis C
Pre-test counselling, confirmatory test
Make sure that you listen to the patient, their concerns, and elicit questions. If they remember the main points about testing, you do not need to go through all of them. After answering their questions and concerns, you can start out with something like the script below. Be sure not to repeat things that they already told you they know and understand well. Expand more on the points that they asked you about.
This script assumes that a person has come individually, and will be tested and treated at the same facility. You should adapt the suggested script to situation, the context, and the project.
“The previous test showed that you had an infection of hepatitis C at some time in your life. The test we will do now will tell whether you still have that infection. If the test shows that you do still have an infection, we will do more tests to find out more details, such as how much your liver has been affected by the infection.
“The infection can be in your blood for years without causing much damage. But eventually there is a high risk of serious damage to your liver that can cause liver cancer or other very serious problems. However, the medicines are very effective, and stop the damage.
“We cannot tell how you have been exposed to hepatitis C, or how long ago.
[If there is a household testing and treatment protocol, and household has not yet been tested:]
As you have been exposed to hepatitis C, it is possible that others in your household have also been exposed. I recommend that all the members of your household get the rapid test for hepatitis C virus, like you had.
“Your hepatitis C test results are confidential. We will not release your results without your permission. You can tell whoever you like, but you should not ask other people their results.”
You should also explain the testing procedure, and tell them how long it will take to get results. As them how they wish to be notified of results. They may not be thinking of confidentiality, so you must. Double check with them if their notification method is private. If their household is to be tested, let them know how to get the test.
back to Counselling
Post-test counselling, confirmatory test for HCV
Post-test counselling, confirmatory test
This is should be the fourth time that the person has had counselling, so be responsive to their knowledge. However, this may also be the last time they receive counselling, and not every person has received all the counselling. The counselling should be adapted to the person’s situation, and to what you have to offer them.
First, ask for any questions or concerns. Then tell the results, and ask for any questions again.
For negative results, at a minimum, explain:
The test is negative, and that means that you do not have active hepatitis C infection. The previous test showed that you have been exposed at some time in your life. The test cannot show how or when. Your immune system cleared the infection, and the virus is gone.
[If useful, make a comparison to a cold or flu.]Even though you got over the infection before, you can get it again. Hepatitis C is one of the viruses that you can get more than once. You are not immune to hepatitis C, and you still need to avoid [fill in main risks from your context].
Before saying good-bye, ask for any questions or concerns again, and give a way to contact an appropriate person, place, or service in case they have questions in the future.
For positive results, the content of what you say will depend on what you can offer. At a minimum:
The test is positive, which means that you have an active hepatitis C infection.
[If your testing method allows you to say whether it is a recent or chronic infection, tell them which. If recent infection, follow your organisation’s protocol about whether to treat or to wait to see if the person clears the infection.] The following assumes chronic infection.
Do you have any specific questions or concerns you would like to talk about?
Your health is not in immediate danger, but hepatitis C virus can gradually damage the liver. There are medicines which are very good and have few side effects. Most people are cured in a few months. Your doctor will give you more details about the medicines. You should be avoid alcohol, because it can speed up liver damage.
The next step is to get some more tests which will give the information needed to make some decisions about treatment.
Now is the time to give the person more details about hepatitis C and its progression. How much and in what detail you will explain will depend on their knowledge, your knowledge, and the roles in your organisation.
Let the person know all the next steps according to your protocol. They should know:
1) where they need to go,
2) how many steps and the timing (further testing, results, consultations, initiation),
3) who will provide what for them,
4) the costs for any steps of the process.
Make sure that they understand all the steps and the reasons for them. Have them available in writing, but know that some people may not wish to take a paper. Make sure they know who to contact if they have concerns, questions, or need to change any appointments. Before saying goodbye, make sure they are not distressed, and that they know what resources there are for their support, such as patient groups.
The patient will get information another time from the prescribing provider when they start treatment. At that time, they will get more information about medications they may be taking and liver health, the results of further tests, and other matters. The aim of pre- and post-test counselling is partly to give information to all test-takers, so they can protect themselves and others, and to reduce stigma. It also prepares those who are positive to have a basis for clear understanding of their treatment and health prospects in the long term. With a solid knowledge basis from graduated layers of counselling, a patient will understand the treatment better, be able to better inform the treatment provider of their particular circumstances, be able to ask better questions, and better able to advocate for themselves.
On this page: 1. Testing ・ 2. Counselling